Exploring the Long-Term Effects of Rheumatoid Arthritis on the Body
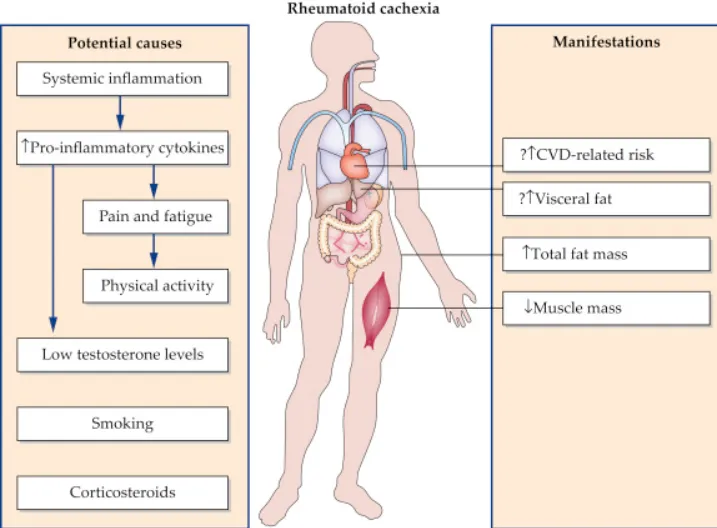
Rheumatoid arthritis (RA) is a chronic autoimmune disease that primarily affects the joints. However, its impact extends far beyond the joints, affecting various systems throughout the body. Understanding the long-term effects of RA on the body is crucial for patients and caregivers alike, as it sheds light on the comprehensive management and treatment of this complex condition.
Contents
The Joint Deterioration Cascade
RA is characterized by inflammation of the synovium, the lining of the joints. Over time, this chronic inflammation leads to irreversible damage to the cartilage, bone, and surrounding structures. The joints become swollen, stiff, and painful, impairing mobility and function. Without proper management, RA can progress rapidly, causing deformities and disability.
Systemic Involvement: Beyond the Joints
Beyond joint inflammation, RA can impact multiple organ systems, leading to a range of complications:
Cardiovascular System
RA is associated with an increased risk of cardiovascular disease. Chronic inflammation contributes to the development of atherosclerosis, increasing the likelihood of heart attacks and strokes. Additionally, inflammation can affect the heart muscle and the lining of blood vessels, leading to conditions such as pericarditis and vasculitis.
Respiratory System
RA can affect the lungs, causing inflammation of the lung tissue (interstitial lung disease) or the lining of the lungs (pleurisy). These complications may result in symptoms such as shortness of breath, coughing, and chest pain. Over time, lung function may decline, impacting overall respiratory health.
Nervous system
Rheumatoid arthritis (RA) not only affects joints and organs but also the nervous system, leading to neuropathy symptoms such as tingling, numbness, and weakness. In RA, neuropathy can develop due to inflammation or nerve compression from swollen joints or rheumatoid nodules. Untreated neuropathy can lead to complications like loss of sensation and motor function, impacting mobility and quality of life. Recognizing and addressing neuropathy symptoms in Oklahoma City as part of RA management is crucial for minimizing long-term neurological effects and improving patient outcomes.
Eyes
RA can affect the eyes, leading to inflammation of the sclera (scleritis), the outer layer of the eye. Additionally, dry eye syndrome is common in RA patients due to inflammation of the tear glands. If left untreated, these conditions can lead to vision impairment and discomfort.
Skin
Skin manifestations are common in RA, including rheumatoid nodules, which are firm lumps that develop under the skin, typically around pressure points or joints. Other skin conditions associated with RA include vasculitis, ulcers, and rashes. These manifestations can significantly impact a patient’s quality of life.
Impact on Bone Health
RA increases the risk of osteoporosis, a condition characterized by weakened bones and an increased susceptibility to fractures. Chronic inflammation, use of corticosteroids, and reduced physical activity contribute to bone loss in RA patients. Osteoporosis further exacerbates the risk of fractures, adding to the burden of disability and impairment.
Psychological and Emotional Toll
Living with RA can take a significant toll on mental health and well-being. Chronic pain, fatigue, and disability can lead to feelings of depression, anxiety, and social isolation. Coping with the physical limitations imposed by RA can be challenging, requiring resilience and support from healthcare professionals, family, and peers.
Management and Prevention Strategies
While RA presents formidable challenges, proactive management strategies can help mitigate its long-term effects:
- Early Intervention: Early diagnosis and treatment are critical in preventing joint damage and systemic complications. Timely initiation of disease-modifying antirheumatic drugs (DMARDs) can help control inflammation and preserve joint function.
- Comprehensive Care: A multidisciplinary approach involving rheumatologists, physical therapists, occupational therapists, and other healthcare professionals is essential in managing RA comprehensively. Regular monitoring of disease activity, medication adjustments, and lifestyle modifications are integral components of RA management.
- Lifestyle Modifications: Adopting a healthy lifestyle, including regular exercise, balanced nutrition, smoking cessation, and stress management, can help improve overall well-being and mitigate the impact of RA on various organ systems.
- Patient Education and Support: Empowering patients with knowledge about their condition, treatment options, and self-management strategies is crucial in promoting active participation in their care. Support groups and patient advocacy organizations can provide invaluable emotional support and practical advice for coping with RA.
Conclusion
Rheumatoid arthritis is a complex and multifaceted disease that can have far-reaching consequences on the body. Beyond joint inflammation, RA affects multiple organ systems, leading to a myriad of complications and comorbidities. However, with early intervention, comprehensive care, and proactive management strategies, the long-term effects of RA can be mitigated, enabling patients to lead fulfilling and productive lives despite the challenges posed by this chronic condition.